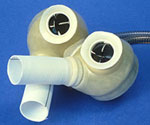
In 1987 I was working for the local hands-on science museum, Discovery World, and part of my job was to beg companies to donate material to our cause. This was not really a task for which I was a natural choice – I am not really a salesman, and not a fund-raiser. As a matter of fact, due to internal politics I was forbidden from fund raising; I could only ask for “stuff.”
We were working on the “Health Is Wealth” exhibit, a compendium of stations, 23 in all, covering many aspects of whole-body health. We were looking for a blockbuster addition to this exhibit, and as artificial heart research was very much in the zeitgeist I was tasked with trying to get one. Being a novice and an innocent, I called up Symbion, the firm formed by Robert Jarvik, the inventor of the first practical, implantable, total artificial heart (TAH); the Jarvik 7. “Hi, This is Nic Bernstein calling from Discovery World museum in Milwaukee, Wisconsin. I am calling because I see that you have just removed a heart from a local man, and we were wondering if we could get that unit to display in our new exhibit…”
Yes, I actually made that call, and the response I received was much more polite than you might expect. “Well, we have received that heart from the implanting hospital, Saint Luke’s, but under FDA guidelines we have to disassemble the heart, test the components and then return the whole works to their labs.”
“Oh, well I guess that makes sense… Have you got any suggestions for me as to how I may be able to get one? We would really like to exhibit one, and seeing as a local man just had one, and local interest is high, it just seems like the time is right.”
“I tell you what, we cannot give you one, all of our hearts must go to an FDA approved transplant site. But, I can tell you this: There are two sizes of hearts, small, for women, and large, for men. Turns out that the large is really too large to implant into anyone’s chest cavity, so we are only using the small ones. St. Luke’s has a large one that they ordered for training. It can never be used, since it is too big, and since it hasn’t been used, they don’t have to return it to us or the FDA, and they need to purchase a new, small unit to train with. You should ask them.”
The next call I placed was to the communications director at St. Luke’s. “Can you give us that training heart that you have? I understand that you cannot implant it, and it would just go to waste otherwise…” I asked. “Tell you what, Nic, I am going into a board meeting right now, let me see what I can do.”
It was all that she would say, and nothing was promised. I put down the phone and waited…
Two hours later the phone rang and it was the communications director form St. Luke’s. “If we were to give you the heart, just how would you exhibit it? How would people see it? I have ten minutes and then I have to get back into the meeting.” she said.
I was stuck cold. I hadn’t thought it through this far… “Well, what we would like to do is have a display where the visitor would place their finger into the plesthysmograph that you gave us, and they would see their pulse on the heart monitor you gave us, and then the artificial heart would start to beat in synchronization with their own.” I offered. I was really loading up the stables on this one…
“Okay, I think I can sell that,” she said, “I’ll call you back in half an hour.” I was both proud and scared out of my wits. I waited, and worried about what I would say to Eric, my engineer.
She called back in 40 minutes and said, “You have your heart! Make us proud.”
Shit! Now came the hard part.
I made the long trek down the hallway to the lab, and sidled up to Eric at his bench. “I have just had a very interesting conversation with St. Luke’s and I have to tell you about it,” I started. “They are going to give us a Jarvik 7 artificial heart.”
“Cool!” said Eric.
“But, I told them that we would make it do this…” I said, and went on to explain to Eric what I had told the PR woman that we would do.
Eric thought about what I said, and then he said something like “Well, I guess we need to find out about it’s control circuitry.”
The next day I called back to Symbion and asked my contact if he could put me in touch with someone in the engineering department. “I heard from Bridget that you got the practice heart!” he shared, “Good play. Talk to this guy…” and he gave me a name and number. A few minutes later I was speaking to the head engineer. I explained what we wanted to do, and asked if we could get plans for their drive systems. It wasn’t going to be that simple.
The original Jarvik 7 heart was a bulky, and balky, device which was pneumatically driven. The control cabinet was about 4 feet tall by 2 feet wide, and housed an air pump, and a pair of drive assemblies. The drive controls had a pair of dials on their face, one of which controlled pulse rate and one of which controlled the duty-cycle; the ratio between systoli and diastoli — the amount of time the heart pumped in versus out. These values were hard coded, so to say, and did not vary. In other words, if you had a Jarvik 7, you would get a dialed in pulse rate, say 72 beats per minute, and a dialed in duty cycle, and that was that. There was no variability, there didn’t need to be.
I was crestfallen. How were we going to synchronize a Jarvik 7 to the visitor’s heart if the control unit was fixed? Well, we soon discovered that was not going to be an issue as we were not getting the control unit, just the heart. I called the engineer again. “Well, I can tell you that you need this amount of pressure to cycle the heart, and that you need this amount of resistance, and back pressure, but beyond that, I don’t know what to say…” “We want it to track the visitor’s heartbeat” I said. “Well, if you get that to work, we would love to see what you’ve done, ’cause that’s way beyond anything we’ve done.” Oh goody.
Well, long story short, Eric did it. He built an analogue computer which performed quadrature upon the output of the plethysmograph and drove the parallel pneumatic drives to the heart. A week or two later our heart arrived, and we had to put it to the test. A heart pumps against a load; in the body that load is provided by the arteries and the miles of blood vessels and veins. In our test, as we had yet to construct our hydrostatic tanks, we simply immersed the heart into a bucket, “more than six inches deep,” we were told. I handed the heart to Jerry, a Bible thumping shop guy, after first connecting it to the pneumatic tubes. I placed the plethysmograph onto my finger and Jerry plunged the heart into the bucket, and we turned on Eric’s drive unit. The heart started to pulse, and Jerry yanked his hand out of the water and ran to the other side of the shop spewing oaths in his wake. I grabbed the heart to keep it from surfacing, and had the most bizarre experience of my life. I was holding my own heart under water, it seemed, as it beat in perfect synchronization with mine, and with a firm and resolute rhythm.
We had done it! We, a small and underfunded science museum in Milwaukee, Wisconsin, had designed and built the most advanced artificial heart drive system in the world! We made minor adjustments to the system after that, and ultimately we were unable to allow the visitor to experience that eerie, out-of-body, sensation that I had of holding my own heart in my hands, but we had to protect the heart.
We did send all of our design materials off to Symbion. We never heard if they used any of them, but in the ensuing years the dream of a totally-implantable artificial heart (TAH) gave way to the more pragmatic ventricular assist device, the intra-aortic balloon pump, and similar heart pumps, assists, etc. All of these new generation of heart savers share the quality of tracking the patient’s own heart rate, systoli and diastoli. Whether or not our work was used, we laid the path.
Tonight, as I write this, my friend Tom is having a pair of ventricular assist devices installed into his chest cavity. If all goes well they soon will help his heart, his scarred and stricken heart, and pulse and pump blood though his veins. I do not claim anything in this, but I would like to think that in our own way, due to our own imperatives, we showed a generation of heart surgeons and clinical engineers that it was important to consider the patient’s own heart, their own pulse, when designing the systems by which we would keep them alive.
Mostly, however, I have to write this because I really want Tom to live and I have to do something with my fingers while he lays on that operating table and has this generation’s best and brightest install a piece of machinery into his chest to keep him alive long enough for me to tell him to his face how important he is to me.